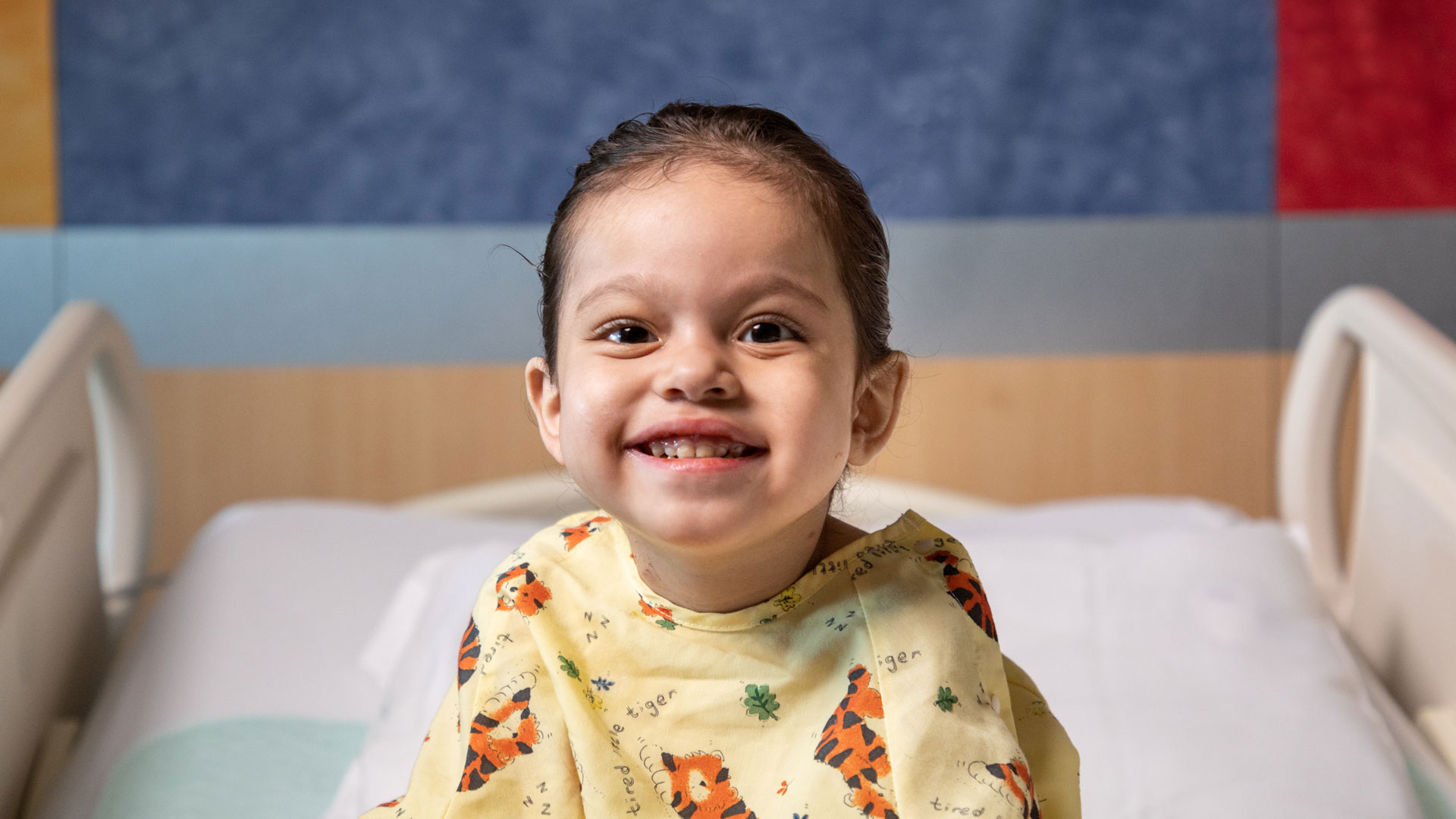
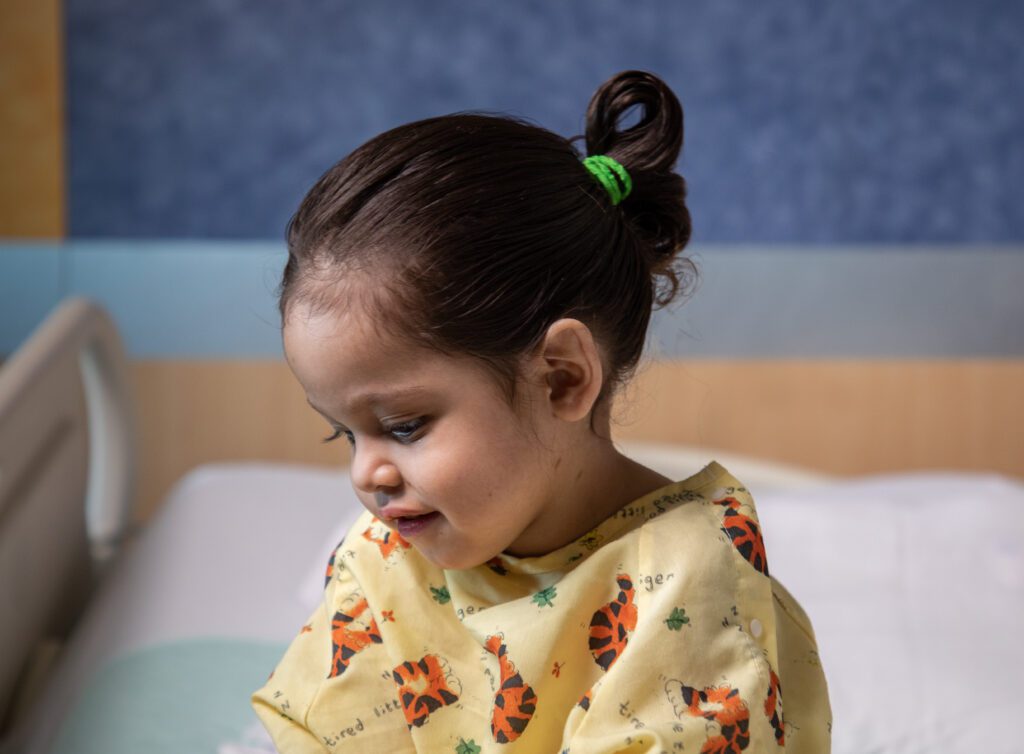
It was August 5, 2022, and Namiko was staying on the seventh floor of Phoenix Children’s Hospital. That day, she was a ball of energy—giggling, playing, snuggling with dad. Her face was radiant; she looked healthy and full of life. So when her family shared her story—and spoke of a time when life was drained from her—it became clear that Namiko was a child of radiance and resilience.
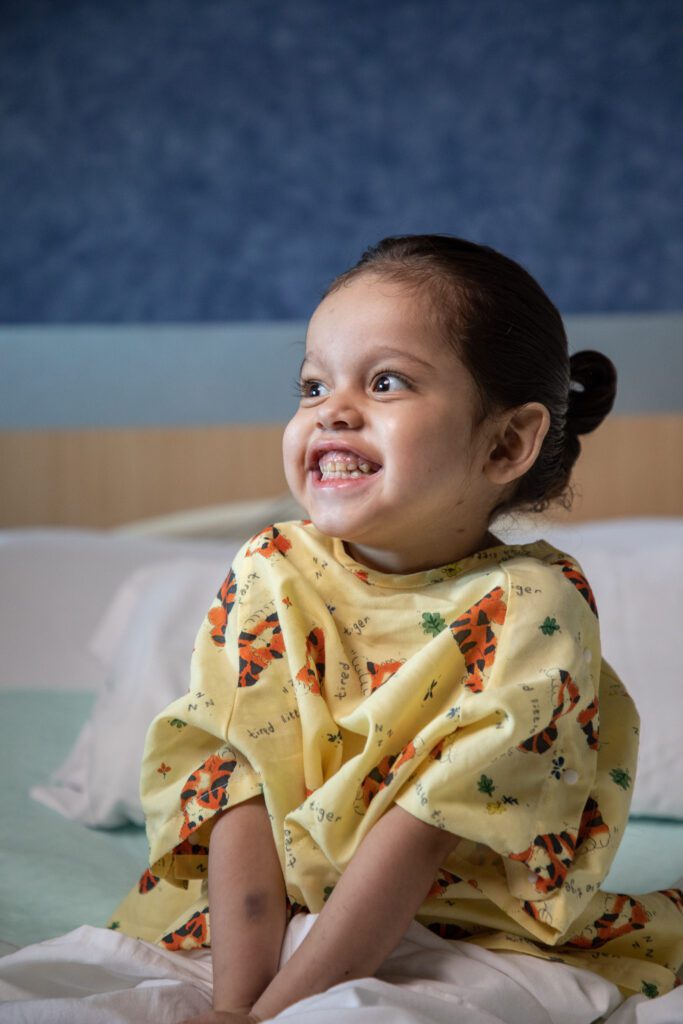
The color of … lemon juice?
Vanessa noticed her baby’s skin was the color of lemon juice early in the summer of 2019, when Namiko was 2 months old.
At first, she thought Namiko needed more sunshine. But she decided to get testing done to be sure. To Vanessa’s surprise, bloodwork revealed a dire situation: Namiko’s bilirubin levels were skyrocketing. Normal levels for children are one milliliter per deciliter of blood. Namiko’s were at 14.
Bilirubin is a yellowish waste product that binds to bile, a fluid secreted by the liver. It is removed from the body via the digestive tract. Instead of being excreted normally, Namiko’s bilirubin was leaking out of her liver and into her bloodstream, causing her skin to yellow, a condition known as jaundice.
“At first, the doctors did not know why,” Vanessa says. “They ran all kinds of tests. They did ultrasounds. Then they found out from a scan that she has biliary atresia.”
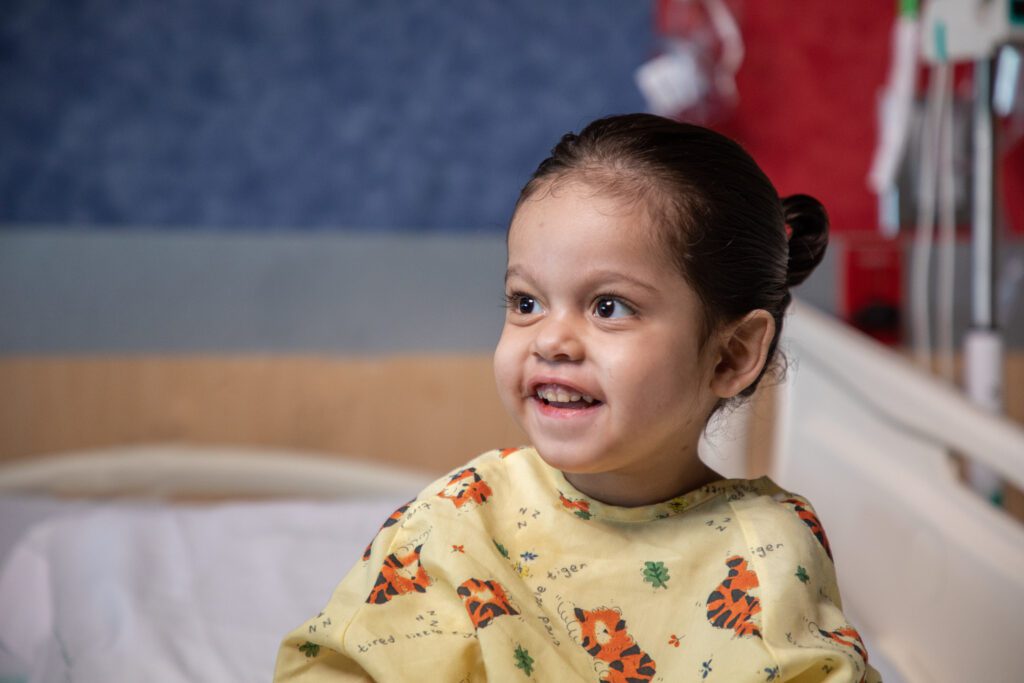
In children with biliary atresia, the bile ducts, a network of tube-like structures that carry bile from the liver to the small intestine, are blocked due to scarring or improper development. As a result, bile cannot flow to the small intestine where it helps to break down food. Instead, it builds up in the liver, causing damage.
About 300 babies are born with biliary atresia each year in the United States. Though the disease is rare, experts emphasize, it is the most common cause of liver-related death in children. Without liver transplantation, very few children with the condition live past 2 to 3 years of age.
“When I heard the news, I could not stop crying. I couldn’t even process everything,” Vanessa says.
A temporary solution
The day after her diagnosis, Namiko underwent a Kasai procedure at a hospital in her hometown of Tucson, where her blocked bile ducts were replaced with a segment of her small intestine.
Normal restoration of bile flow occurs in one-third of children who have a Kasai procedure. The remaining two-thirds will need liver transplants—about half soon after the procedure and the other half later in life.
After surgery, Namiko spent two weeks in the hospital recovering before she went home. She headed back to the hospital often for check-ups. Vanessa cannot recall many sweet memories of motherhood during this time. “We were almost constantly in and out of the hospital so it’s kind of hard. I can’t really think of anything,” she explains.
At 3 months, Namiko was referred from her hospital in Tucson to Phoenix Children’s because its Hepatology Program provides services that aren't offered anywhere else in the state. At the time, she was still jaundiced. “I thought she was going to be good after the procedure. I was pretty much trying to convince myself,” says Vanessa.
And then came a moment of relief. Namiko’s bilirubin levels improved—a reading of three mL/dL. This was a result of the procedure and the 13 medications she was taking. “I was ecstatic. I had a positive outlook,” Vanessa says. For the first time, her daughter’s personality was emerging; she was becoming a talkative, playful baby. But Vanessa’s joy would soon turn to crushing fear.
Top of the list
Vanessa and George, Namiko’s dad, remember October 5, 2020, clearly.
Namiko was playing with dad in the living room and began to crawl towards mom in the kitchen. Halfway there, she collapsed. George quickly picked her up and walked towards Vanessa.
Seconds later, the kitchen was covered in sprays of blood.
Vanessa called 911. But she hung up because she believed it would take the ambulance too long to arrive. “I was freaking out. I couldn’t think,” she recalls. As the family drove to the emergency room, Namiko was nodding in and out, expressionless in the back seat.
Scarring on her liver (caused by the buildup of bile) had prevented blood from flowing through the organ. It rerouted into smaller vessels that aren’t designed to carry large amounts of blood, including the veins that lined Namiko’s esophagus. Burdened by the influx, her esophageal veins “ballooned and exploded,” forcing her to cough up blood.
Namiko was admitted to the hospital where she continuously bled from her esophagus and gastrointestinal tract for a week. Doctors' initial efforts to control the bleeding were futile. They administered a large dose of vasopressin as a last resort—without this medication, Namiko would likely bleed out.
Externally, Namiko was “out of it,” says Vanessa. “Her eyes were rolling back. She would look your way, but you could tell she wasn’t there. It was pretty much life or death in that moment.” George adds, “I didn’t want to lose her. She’s my first baby.”

Doctors placed Namiko on the transplant list at status 1A—the top priority. Her family waited for a match. A sliver of hope arose when a liver became available during Christmastime that year. But it turned out to be false hope—the liver wasn’t the right size.
Miraculously, seven blood transfusions and many medications later, the little fighter recovered. Her bleeding stopped. She remained on the transplant list, but she was no longer 1A. And she lived a fairly normal life for a while.
A message from one little warrior to other young fighters
Namiko received her new liver on July 27, 2022. It was a gift she had been waiting on for almost three years. The next day, doctors had her out of bed, working to rebuild her strength. She was discharged from the hospital two weeks later.
During her hospital stay, Namiko found comfort in a special teddy bear with an IV and a PICC line in its arm, a bandage wrapped around its belly, and a drain in its side—a tool Child Life specialists used to help her understand why there were tubes and gauze on her body after her transplant.

Vanessa says, “We told her straight up, ‘You have a new liver, and we are going to take good care of it.'”
Today, Namiko's liver numbers are normal for the first time in her life, and her parents describe her as “more hyper and sassy than ever before.” Namiko affectionately calls her scar a “smiley face”—the eyes are where her abdominal drains once were, and her incision forms the mouth.
When asked what she would say to other sick children, she exclaims, “You can do it!”

Namiko, like all the young patients in Phoenix Children’s care, is the face of strength, resilience and courage. Bring hope and healing to patients like her today.