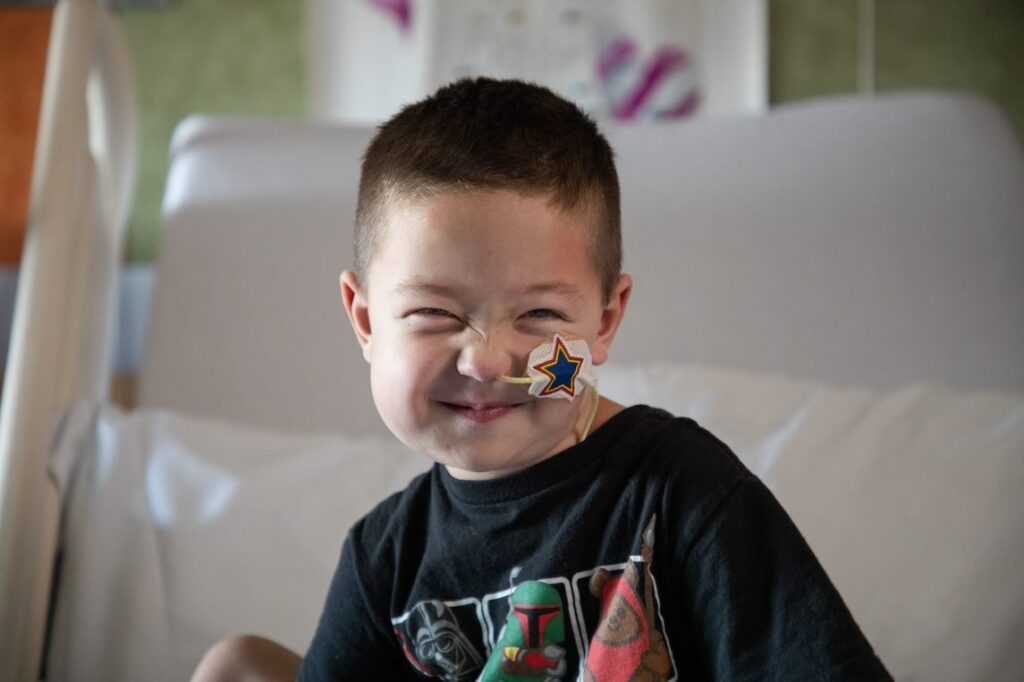
Andrea was a happy 11-year-old kid when she and her family received devastating news—she was in heart failure and likely wouldn’t live to see her teenage years. Even worse? Andrea’s older sister, Adina (not pictured), was also in heart failure. Both girls had been born with a life-threatening condition called hypertrophic cardiomyopathy, and both would need heart transplants.
When Andrea’s parents got the call that there was a donor heart ready for her, Andrea’s feelings were confusing to her. She recalls being relieved but also scared to undergo the operation first, before her sister, and guilty that a match hadn’t been found yet for Adina.
“A heart transplant is an extraordinary lifesaving and life-changing experience for a child with a serious heart condition,” says Sarah Anais Mejia, PhD, a psychologist who works exclusively with heart patients at Phoenix Children’s. “Everyone calls it a gift, but we don’t really use that word for our patients. It’s often more complicated than that.”
Complicated, indeed.

Andrea struggled to balance feeling both grateful for her new heart and grief for the donor family who lost a loved one to make her new life possible. She battled depression and hopelessness. Her mental health declined, and she turned to self-harm.
But it was the steadfast support of her family—including Adina, who received her own new heart shortly after Andrea—and the expertise of Dr. Mejia that helped Andrea begin to heal. Together, they worked to untangle the complicated emotions surrounding her transplant and to build healthier coping strategies. Even today, the two continue to meet for regular check-ins.
“Phoenix Children’s felt like a safe space to express myself,” Andrea says. “They have so many resources to help you when you need it, and the doctors are amazing. They helped so much with my mental struggles. I’m thankful I got to receive care here.”
CARE WITHOUT SILOS
Health care isn’t only about treating the body. Saving lives doesn’t happen exclusively in the operating room, and recovery isn’t solely dependent on prescribing the right medicines. And supporting patients goes beyond the individual. At Phoenix Children’s, care is a spectrum that prioritizes mental health with physical health, and casts a wide net to encompass patients and families.
“Here, we care about the health of the whole child, as well as the health of the whole family,” says Carla C. Allan, PhD, division chief of psychology and the Hagenah Family Endowed Chair in Psychology.
Dr. Allan’s “whole child, whole family” philosophy drives her collaboration with a team of mental health professionals who support children across the Phoenix Children’s system—from routine care to the most complex medical journeys. What does this look like? For Dr. Allan, it’s a strategic series of meaningful, evidence-based—and early—interventions.
“Traditional models of mental health care are that you wait until [a patient] is at crisis,” Dr. Allan explains. “What’s innovative in this space is that we’ve built screening processes universally throughout the health system, so we can catch kids earlier. The goal is not to meet them at the crisis point, but before.
“This represents a real opportunity for us to get ahead of it and serve kids who might otherwise go unrecognized as needing help,” Dr. Allan says.
A SYSTEM THAT SEES THE WHOLE CHILD
Under Dr. Allan’s leadership, meaningful mental health intervention at Phoenix Children’s manifests in a suite of behavioral health initiatives that address a continuum of care. The goal: Position young patients, their families and caregivers for happy, healthier lives in the long term.
One such program embeds compassionate mental health experts, such as Dr. Mejia, the psychologist who shepherded Andrea through her heart transplant, within various specialties. To date, there are nine specialists embedded within five specialties. Philanthropy continues to expand this model, including a recent endowed gift that will support a dedicated psychologist within the pain management program.
These psychologists and psychiatrists support patients and families at every stage of care—from routine visits to life-changing diagnoses—helping them navigate the emotional complexities of illness while bringing an unprecedented level of knowledge and nuance to each patient’s unique situation.
- Here, we care about the health of the whole child, as well as the health of the whole family.CARLA C. ALLAN, PHDDIVISION CHIEF OF PSYCHOLOGY AND THE HAGENAH FAMILY ENDOWED CHAIR IN PSYCHOLOGY
“Creating a broad spectrum of behavioral health care is the new frontier,” says Julia A. Soto, Phoenix Children’s Medical Group administrative director. “Dr. Allan’s leadership and clinical expertise have built this very new frontier of embedding providers in the specialties where children are already coming and receiving care. To have that holistic care with both your medical specialist and your trusted behavioral health provider is unlike previous ways of operating.”
Another crucial intervention includes the donor-funded Suicide Prevention Program.
Suicide is the second-leading cause of death for Arizona children 10 and older, according to the Centers for Disease Control and Prevention. Phoenix Children’s treats as many as 45 patients a day while they are on a mandatory hold for suicidal ideation or waiting for an opening at an inpatient behavioral health facility. The average age of patients coming in with suicidal ideation is 12, but Phoenix Children’s has treated children as young as 5.
All of which is to say: Standard methods for treating mental health issues are not as effective as they could be. That’s why the Suicide Prevention Program screens for suicidal ideation across all Phoenix Children’s outpatient, rehab and medical specialty clinics, as well as across inpatient medical floors. So, for example, when a child visits a Phoenix Children’s clinic for any reason, such as a wellness visit, an eye exam, even a sports medicine appointment, they are given a mental health screening survey. Responses that reveal risk prompt an immediate connection to a mental health therapist before the patient leaves the exam room. The therapist evaluates the child’s mental and emotional state to ensure their safety and determine appropriate next steps.
“Phoenix Children’s has prioritized this as a critical area of health,” Soto says. “And because of that, families do not receive a bill for the screening or immediate intervention. We’re not charging for this care. Caring for kids in all ways is just part of the fabric of who we are and what we aim to do.”


The Suicide Prevention Program launched in 2022 thanks to a philanthropic gift from Chris Koch and Carlisle Companies Incorporated and is now operating across all outpatient clinics, as well as inpatient medical floors. To date, the program has launched 188,000 screenings, identifying over 3,600 kids at risk for suicide. The good news: All these kids had access to real-time interventions and care, and were immediately able to talk directly to a therapist.
Moving forward, the hope is that the Suicide Prevention Program will not only have a profound effect on families in crisis, but also that it can be used as a model for other programs across Arizona and nationally.
EXPANDING THE CIRCLE OF CARE
Additional intervention-based behavioral health initiatives spearheaded at Phoenix Children’s include:
-
- Center for Resiliency and Wellbeing, which helps families address life stressors so that they can better prioritize their medical and mental health care.
-
- Phoenix Children’s Bridge Clinic, a post discharge program where patients meet with a Phoenix Children’s behavioral health provider as often as necessary—sometimes daily—as a “bridge” while long-term care with a community pediatric provider is arranged.
-
- A maternal fetal program that offers Day 1 support—i.e., right at the birth of the baby—for parents and caregivers who’ve been given a tough fetal diagnosis.
-
- A program for neurodiverse children, who often avoid lifesaving medical care because of their heightened sensitivities.
-
- Bullying group therapy, which leverages Phoenix Children’s internal resources to offer group therapy that includes skill-building activities and strategies to address bullying.
-
- Homeless Youth Outreach, a program that provides no-cost comprehensive primary and preventive health care and embedded behavioral health care via three mobile medical units and three fixed-site clinics.
-
- Caregiver support groups, which provide a safe, guided environment for parents and caregivers to share experiences, build coping strategies and receive emotional support while navigating a child’s medical or behavioral health challenges.
-
- An Eating Disorder Clinic that offers treatment and ongoing care for children and adolescents with eating disorders, combining medical monitoring, nutritional guidance and behavioral health support.
-
- Mind, Body, Breath Groups that teach children and adolescents mindfulness and breathwork to manage stress, regulate emotions and support overall mental well-being.
These innovations in the mental health space are integral for building a healthy community here in Arizona and the Southwest, yes—but the outcomes can reverberate nationwide.
“When you couple universal screenings, like those in the Suicide Prevention Program, with a series of evidence-based interventions,” says Dr. Allan, “you can keep kids out of those higher, more costly and challenging levels of care.”
Adds Soto: “As we pilot, build and scale these programs to become as sustainable as possible, and for Dr. Allan to be able to research the outcomes to prove that these work to keep kids out of crisis, we want to share the information. This is not something Phoenix Children’s is copyrighting. We’re ready to share to impact the health of all children.”
THE POWER OF WHAT’S POSSIBLE
As for the future of pediatric mental health—for children facing complex medical diagnoses and for those navigating everyday struggles alike—the groundbreaking work unfolding at Phoenix Children’s leaves Dr. Allan hopeful.

“I’m always hopeful,” she says. “We should all be hopeful. This next generation of kids, for all the challenges they have, are smart, they are kind, they are compassionate, they’re connected, they have passion. This is a good generation. I think they just need a little bit of support when they hit a bump in the road—and that’s what we’re here to provide. We want kids to be engaged with our health system, not to turn away from it.”
Kids like Allyson.
When the teen received a diagnosis of acute lymphoblastic leukemia at the end of her freshman year of high school, her life changed. Her second home soon became Phoenix Children’s Center for Cancer and Blood Disorders, where she underwent three years of treatment, a draining experience that not only took a physical toll but a mental one as well.
“I don’t think I could have grasped the reality of what was about to come,” Allyson remembers.
Grappling with a sea of emotions, trying to understand her diagnosis, adjusting to the drastic changes of her day-to-day life and facing the uncertainty of her future triggered crippling anxiety and fear in Allyson.
MENTAL HEALTH BY THE NUMBERS
A National Challenge
- 1 in 7 U.S. youth ages 6-17 experiences a mental health condition each year.
- Suicide is the second-leading cause of death among youth ages 10-14.
- 50% of all lifetime mental illness begins by age 14, and 75% by age 24.
Source: National Alliance on Mental Illness

Statewide Stats
- 6,504 children ages 0-17 visited a hospital in 2022 due to suicide attempts or suicide ideation; 46 children in that same age group died by suicide.
- In 2021, Arizona’s rate of suicide was 35% higher than the national average per 100,000 people.
Source: Arizona Department of Health Services

Phoenix Children’s Stats
- Every day, an average of 7 children visit Phoenix Children’s emergency department because they wish to harm themselves or others.
- 12 is the average age of children seen at Phoenix Children’s for suicide ideation.
But it was her psychologist—a specialist embedded in the Center for Cancer and Blood Disorders as part of Dr. Allan’s behavioral health initiatives—and Allyson’s Child Life team who supported her medical needs by caring for her mental well-being, giving her tools to manage her feelings while also helping her build coping skills that would serve her, and others, for the rest of her life.
Allyson continues to receive treatment today and is a beacon of hope for those around her. She shares her experiences with other patients and families to help them understand the process—and to make them feel less alone. Thanks to Phoenix Children’s commitment to integrating medical and behavioral health care, Allyson is surviving. And, more importantly, thriving.
“If I could go back and talk to my past self when I first got diagnosed,” Allyson says, “I would tell her that this is just the beginning. You’ll eventually get through this. All the sleepless nights and the pain and the thinking that you’re not going to make it—it passes. You are going to make it. And something beautiful will eventually come out of it.”
At Phoenix Children's, these moments shape futures and save lives, thanks to your support.